Household health systems: community health workers for Universal Health Coverage

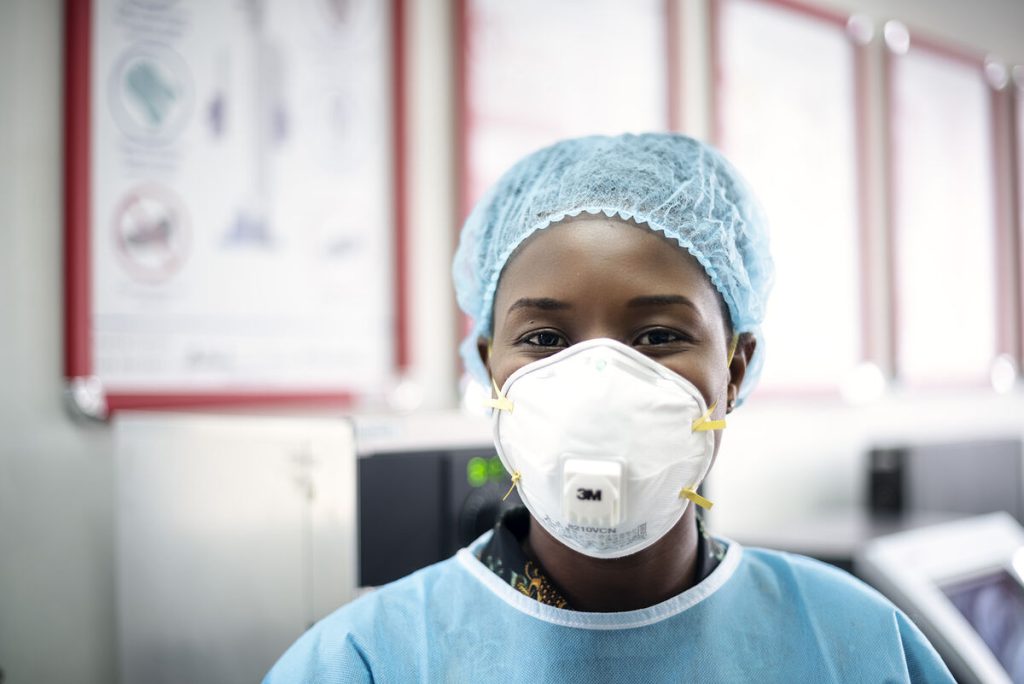
Maureen is one of Kenya’s community health workers (CHWs), the frontline providers who deliver essential healthcare where hospitals and clinics are often too far, too costly, or too overstretched. Her story captures both the promise—and the fragility—of community health systems.
One day, Maureen visited a household where a child was showing signs of malaria. She knew what to do. She had been trained to recognise the symptoms. But she lacked the kit to confirm the diagnosis.
Her only option was to refer the child to a distant health facility, where the family would face long travel, long waits, and higher costs. Care that could have been provided safely in the community was delayed.
This gap matters more than ever. In Kenya, non‑communicable diseases (NCDs) are now the leading cause of death. “These are diseases that start in the community, because lifestyle is set by communities,” said Dr Joel Gondi, Director of Primary Health Care at Kenya’s Ministry of Health. “That is why primary health care—and community health workers—are at the centre of our strategy.”
The Community Health Units for Universal Health Coverage (CHU4UHC) programme exists to close that gap. Led by the Kenyan Ministry of Health and implemented by partners including Amref, the programme supports CHWs to be trained, equipped, supervised, digitised and remunerated, so they can deliver care where it is most effective: at home.
When that support works, the results are profound.
Maureen recalled visiting a pregnant woman whose blood pressure was dangerously high. Because she had the right tools and training, she made an immediate referral and followed up closely after the woman returned home.
“The baby was born healthy—and they named her after me,” she said, smiling.
Stories like this are why Kenya is becoming a global leader in professionalising community health workers. With continued flexible, long‑term funding, CHU4UHC is showing that universal health coverage does not begin in hospitals—it begins in households, with trusted, supported community health workers at the centre.