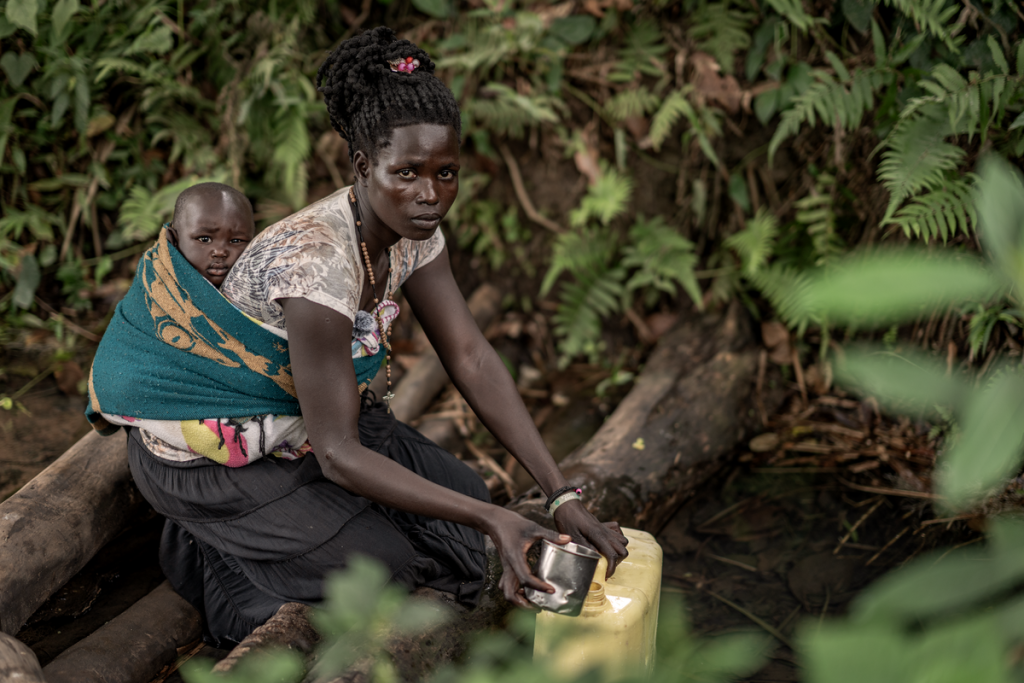At the end of January 2025, vital US Government funding for global health programmes was suddenly frozen.
In the weeks and months that followed, other nations announced cuts to their own foreign aid budgets, which are known as Official Development Assistance (ODA). The UK announced a cut to its ODA, the latest in a succession of cuts since 2020, bringing it to the lowest level it’s been in a decade.
These aid cuts hit health programmes hard, with the impacts felt most deeply in communities which relied on the health services they funded.
One year of aid cuts impact
One year on, people are struggling to access the health services that were once provided in their communities. This means fewer people are able to access the healthcare that they need – a core human right.
We recently connected Hester Nyasulu, Country Director, Amref Malawi and Moshin Ranathunga, Head of Programmes, Amref South Sudan with a group of Amref UK partners and supporters in a discussion that centred on the diverse impacts of the aid cuts in Malawi and South Sudan.
They gave an open and honest view of what is happening to people because of the aid cuts. And, they prompted a discussion on what the priority areas for urgent funding are in Malawi and South Sudan. Here’s the highlights of the conversation.
Malawi needs integrated family health clinics
More than 80% of people in Malawi live in rural areas. Many of them live more than 20 or 30km from the nearest health centre, a costly journey taking time away from home and work.
Community Health Workers (CHWs) – people trained to provide basic health services and referrals for more complex issues – were supported to provide outreach clinics to remote communities. Antenatal services, routine childhood vaccinations were core services. With the aid cuts, the CHW no longer has all the equipment and medication required to serve their community.

“Now, a community health worker doesn’t have the supplies, equipment, medication that are needed. [They are] just there as a doctor.”
Listen to Hester Nyasulu expand on the impact the cancellation of the integrated family health clinics has had on communities across Malawi.
Clinics that would have provided critical antenatal services now do not exist for most communities. Hester says this means pregnant women are forced to walk for 30km or more to reach care. In the later stages of pregnancy, or if a woman has complications, this is impossible.
“We are now depending on a few resources we have, we are able to reach at least about 50% of this scale. But it’s making us not sleep because we know there are a lot more people who need services out there,” Hester added.

In South Sudan, the aid cuts "were like a switch being turned off"
Since independence in 2011, South Sudan has been heavily reliant on external donor funding of its health system. Historically, this was provided through the UK Government and other European institutional donors. These funds “carried the whole health system” said Moshin Ranathunga, Head of Programmes at Amref South Sudan. As the world’s youngest country, South Sudan had no established system, so external donors helped to set it up and run it.
They paid for the health infrastructure, the salaries of health workers called ‘incentives’, medicine and equipment, fuel for the ambulances. The cuts stopped services “overnight and outright.”
"There are no surgical teams, there are no drugs, there is no medicine, all the equipment is more or less non-functional...A box of gloves (24 pairs) had to last for 3 months. It's next to impossible."
Listen to Moshin explain more about how the aid cuts are reversing progress on health in South Sudan. Amid political conflict, spreading to violence, and brutal cuts, Amref has had to refocus our work on emergency support rather than sustainable systems building.
In the face of the cuts, both Hester and Moshin described how other donors were stepping up to help bridge the gap left by the aid cuts. The message was clear: every little bit helps.
Looking ahead: the new reality
In South Sudan, the situation is fragile and fraught. Moshin reiterated that the urgent funding priorities for Amref’s work, and wider health partners’ work, in South Sudan are the basic essentials: drugs and medications, and surgical staff. They are doing a lot with a little, because of the circumstances in the country, so every piece of help goes a long way.
In Malawi, Hester emphasised the importance of the integrated family health outreach clinics that provide vital health services particularly for mothers and children across Malawi. Support with health financing to build a sustainability plan with the Ministry of Health and a direct injection of resources are also key funding priorities for Malawi.
They left us with the pervasive optimism that powers community resilience and hope.
We do everything in South Sudan with the hope that it will be better tomorrow.
Moshin Ranathunga, Head of Programmes, Amref South Sudan
Sign up to our newsletter to get invites to events like this
By signing up you are agreeing to receive updates on Amref’s work, stories of impact and ways you can get involved. You can opt out at any time.